Cervical cancer is a preventable disease. It is also curable if detected early and adequately treated. Yet it remains one of the most common cancers and causes of cancer-related death in women across the globe. The annual number of new cases of cervical cancer has been projected to increase from 570 000 to 700 000 between 2018 and 2030, with the annual number of deaths projected to increase from 311 000 to 400 000. More than 85% of those affected are young, undereducated women who live in the world’s poorest countries. Many are also mothers of young children whose survival is subsequently truncated by the premature death of their mothers (1).
Few diseases reflect global inequities as much as cancer of the cervix. In low- and middle-income countries its incidence is nearly twice as high and its death rates three times as high as in high-income countries. Proven and cost-effective measures for eliminating cervical cancer exist, but to date have not been widely implemented in regions of the world where the disease burden is highest. To be optimally effective, these measures must be scaled to national levels and delivered using health service platforms that are sensitive to women’s needs, their social circumstances, and the personal, cultural, social, structural and economic barriers hindering their access to health services. Health services that are integrated and people centered, and that respect and uphold women’s rights and dignity, are vital.
Urgent and bold action is needed to scale up and sustain implementation of the evidence-based interventions (human papillomavirus (HPV) vaccination, cervical cancer screening and management of detected disease) for eliminating cervical cancer as a public health problem, but such action must be strategic.
This global strategy to eliminate cervical cancer proposes:
- a vision of a world where cervical cancer is eliminated as a public health problem;
- a threshold of 4 per 100 000 women-years for elimination as a public health problem;
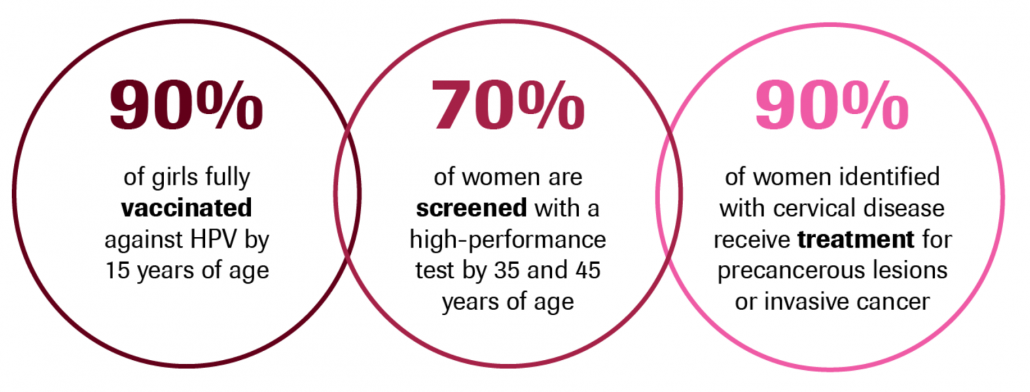
- the following 90-70-90 targets that must be met by 2030 for countries to be on the path towards cervical cancer elimination:
- a mathematical model that illustrates the following interim benefits of achieving the 90-70-90 targets by 2030 in low- and lower-middle-income countries:
- median cervical cancer incidence rate will fall by 42% by 2045, and by 97% by 2120, averting more than 74 million new cases of cervical cancer;
- median cumulative number of cervical cancer deaths averted will be 300 000 by 2030, over 14 million by 2070, and over 62 million by 2120.
The global strategy to eliminate cervical cancer as a public health problem will require:
- political support from international and local leaders;
- coordinated cooperation among multispectral partners;
- broad support for equitable access in the context of universal health coverage;
- effective resource mobilization;
- health system strengthening; and
- vigorous health promotion at all levels.
The interconnected nature of gender and health must stand as the strategic centerpiece of interventions. The strategy must also be open to the exploration and exploitation of new ideas and opportunities, including advances in developing new medicines, vaccines, diagnostics and treatment modalities. In order to achieve its targets, the strategy must embrace innovative models of service delivery and computerized data and information systems, together with new and expanded training methods (for example, using virtual reality simulations) and interventions scaled up to population level (for example, mass campaigns to screen and treat cervical cancer, and surgical camps). Management science and modern forms of communications technology must be integrated into all aspects of service delivery. The market must be reshaped to eliminate cost as a barrier to prevention and treatment in the world’s poorest countries.
The moment has arrived for an ambitious, concerted and inclusive strategy to accelerate eliminating cervical cancer as a public health problem. Elimination is within the reach of all countries. We know what works. The technology and tools exist. We know that prevention and early diagnosis and treatment are highly cost effective. The current focus on universal health coverage demonstrated by the United Nations General Assembly in September 2019 offers a unique opportunity for countries to strengthen interventions for the management of invasive cervical cancer (2).
“Through cost-effective, evidence-based interventions, including human papillomavirus vaccination of girls, screening and treatment of precancerous lesions, and improving access to diagnosis and treatment of invasive cancers, we can eliminate cervical cancer as a public health problem and make it a disease of the past.” Dr Tedros Adhanom Ghebreyesus, Director-General, World Health Organization
Please watch this video short of a full-length documentary on the global Conquering Cancer initiative. The video features inspirational stories from cervical cancer survivors and health care professionals who are looking at the 10-year horizon, and challenging country leaders to take action towards the goal of worldwide cervical cancer elimination by 2030.
More information:
References:
- Mailhot Vega RB, Balogun OD, Ishaq OF, Bray F, Ginsburg O, Formenti SC. Estimating child mortality associated
with maternal mortality from breast and cervical cancer. Cancer. 2019;125(1):109–17. doi:10.1002/cncr.31780. - Resolution adopted by the General Assembly on 10 October 2019. Resolution 74/2: Political declaration of the highlevel meeting on universal health coverage. New York: United Nations General Assembly, Seventy-fourth session; 2019
(https://undocs.org/en/A/RES/74/2, accessed 2 October 2020).
For HCPs only
MC-HR-01710